| |
Editor’s Note: Phase I study of the “gap” |
For many years, our CME oncology group has attempted to utilize educational objectives that bridge what we call “the gap” — the difference between “standard of care” as defined by cancer research leaders and oncologic care delivered by community-based oncologists. In the many audio interviews and CME meetings with breast cancer specialists (BCS) over the years, we have noted a great deal of homogeneity in their approach to patient care. Their practices also generally closely reflect NCCN and ASCO guidelines. There are relatively few researchers in any given tumor type, and these oncologists are frequently interacting together on education panels and in research planning meetings. This results in a continuous informal consensus process.
Community-based oncologists (CBO) are not nearly as connected, and there is much more heterogeneity in their practice patterns. One can argue that for many clinical situations, there are multiple evidence-based options, and perhaps the judgment of CBO is more astute than that of researchers. However, I suspect that many CBO do not have the necessary time to adequately review the available research data on the many tumors they must treat and this is the most likely cause for differences in care patterns.
For this special issue of Patterns of Care, we attempt to quantify the “gap” for a number of common clinical scenarios in the management of breast cancer. In February 2005, 74 clinical researchers who specialize in breast cancer were invited to complete the same case-based survey that was given to 200 medical oncologists randomly recruited from a national mail list six months earlier (see Volume 1, Issue 3 of this publication). Thirty-one of these investigators — most of whom have previously been interviewed for our audio series — completed the surveys (see next page for complete list of respondents).
A number of these research leaders also participated in hour-long follow-up telephone interviews, which were transcribed and edited as commentary for this issue. This issue also includes relevant comments from other researchers that were gleaned from our audio programs.
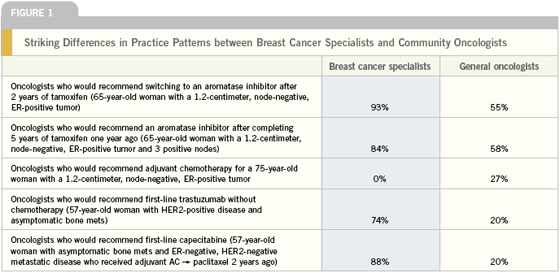
The two sets of survey results demonstrate that while there is general concordance about medical management of breast cancer, there also are a number of clinical situations where significant differences exist between these two groups (see Figure 1, below, for examples).
Perhaps the most interesting finding from the comparison of these two surveys was that the number of breast cancer patients treated by BCS is about the same as those treated by CBO. This occurrence is likely unique in contemporary oncology. Typically, research leaders who specialize in specific tumor types have a great deal more clinical experience with those diseases than CBO do.
For example, I recently interviewed Steven Rosen from Northwestern University for our series in non- Hodgkin’s lymphoma. Dr Rosen has a particular research and practice interest in cutaneous lymphomas, which represent less than 2,000 cases annually in the United States. Every day, he sees patients with these tumors, which are very rare in general oncology practice. This has important implications for education, as practitioners commonly seek “pearls” about caring for patients with these uncommon tumors from specialists like Steve.
Click here to see image
During the interview, we reviewed a number of Dr Rosen’s second opinion cases, and in several instances, there was a marked difference in his recommendation compared to the first. In one case, a patient was recommended to have high-dose chemotherapy with stem cell support, but Steve recommended watchful waiting, an approach the patient continues to take 12 years later without difficulty. While such disparities are uncommon in breast cancer, the enclosed breast cancer survey demonstrates many common clinical situations where significant differences exist between research leaders and oncologists in practice.
From a public health perspective, the most important example relates to switching a postmenopausal woman on adjuvant tamoxifen during the first five years of treatment to an aromatase inhibitor. Two major randomized trials and one smaller one now clearly demonstrate that both exemestane and anastrozole present a much more favorable risk-benefit ratio than tamoxifen to these patients, and one can make the argument that perhaps hundreds of thousands of women are currently receiving treatment that is totally unsupported by breast cancer researchers, and that this exposes them to a 35-40% greater risk of relapse, and a greater chance for serious adverse effects. This is not good and needs to change as soon as possible.
We will be presenting and discussing the data from the surveys at many future live CME education forums so that we can obtain feedback on these trends. We will also continue to track these fascinating practices over time, as new research results emerge and will soon launch a “Phase II study” in this initiative. It will be interesting to follow these trends as new research results emerge.
— Neil Love, MD
NLove@ResearchToPractice.net

Click here to see image
|

