| |
Hormonal Therapy for Metastatic Disease |

Click here to see image
Endocrine therapy for patients presenting de novo with metastatic disease
My goal is to keep a woman on hormonal therapy as long as possible, because quality of life is clearly superior to what it is with chemotherapy. If the patient is hormone therapy naïve, I tend to begin with an aromatase inhibitor, either anastrozole or letrozole. At the time of progression, I often go to tamoxifen and then sequence in exemestane and fulvestrant. If the patient has had tamoxifen, then I go with my nonsteroidal aromatase inhibitor, and then either sequence in fulvestrant or exemestane.
We are participating in several trials that are looking at a loading dose of fulvestrant versus the standard monthly dose. I think it’ll be very interesting to see whether that drug will act differently as the dosing schedule is altered.
— Generosa Grana, MD
We rarely see patients present de novo with metastatic disease. If such a patient does present and they are postmenopausal with ER/PR-positive disease, then I use an aromatase inhibitor based on the current data of increased efficacy when compared with tamoxifen.
— Joanne L Blum, MD
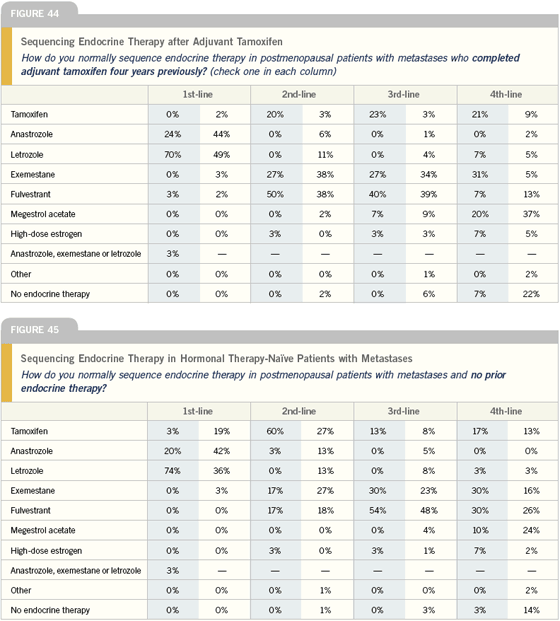
Endocrine therapy for postmenopausal women after adjuvant tamoxifen
Generally, patients are either going to relapse on tamoxifen or after adjuvant tamoxifen. In that setting as well as in the fulvestrant versus anastrozole clinical trials, there is evidence that a proportion of women have a longer response to fulvestrant than to anastrozole when given right after tamoxifen. I have had patients with very long responses to fulvestrant.
I prefer fulvestrant to an aromatase inhibitor after tamoxifen, because approximately 20 percent of patients have very long responses with it in this setting. However, 99 percent of oncologists will choose an aromatase inhibitor after tamoxifen. Fulvestrant is generally being used as third-line.
Despite Trials 20 and 21, most physicians start with anastrozole rather than fulvestrant because of the way the data have been presented. The North American trial data indicates that there was a longer duration of response with fulvestrant; however, the vast majority of oncologists believe fulvestrant and anastrozole are equivalent agents.
Click here to see image
For the last decade, most oncologists have started patients on an aromatase inhibitor — which works. It is hard to argue with something that works. Furthermore, the dose and schedule of fulvestrant is not fully worked out and is under investigation. In fact, some of the current trials of fulvestrant involve three different dosing schedules.
Deciding between fulvestrant and an aromatase inhibitor is also a financial issue. Exemestane, which has 20 percent activity third line, is probably fairly equivalent to fulvestrant. But if a patient doesn’t have prescription drug coverage, a monthly injection of fulvestrant might be more economically appealing than paying $200 to $250 for the aromatase inhibitor.
Click here to see image
So in selecting an endocrine agent for a postmenopausal patient, I generally start with fulvestrant and then switch to letrozole or exemestane. From there, I continue to utilize every available endocrine agent until I’m absolutely convinced that the disease is hormoneresistant and there is no further benefit to endocrine therapy.
— Stephen E Jones, MD
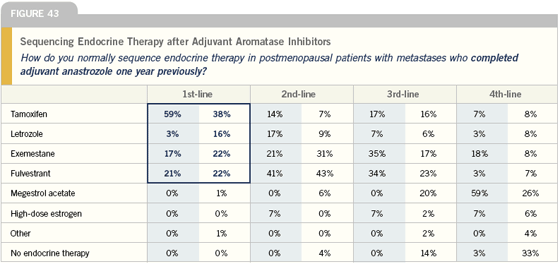
Endocrine therapy for postmenopausal women after adjuvant anastrozole
Previously, patients received tamoxifen in the adjuvant setting, so we would use an aromatase inhibitor front-line in the metastatic setting. Fulvestrant was used second-line, or we could use megestrol acetate, but for many women fulvestrant has a more convenient side effect profile. Now that more women receive aromatase inhibitors in the adjuvant setting, we’re using tamoxifen or fulvestrant as first-line treatment in the metastatic setting.
While I do use fulvestrant, I confess that because of the convenience of oral hormonal therapies, I generally use an aromatase inhibitor or tamoxifen before fulvestrant, but fulvestrant is clearly a reasonable drug to utilize in this setting.
— Harold J Burstein MD, PhD
We are just beginning to see patients who have been treated with two or three years of adjuvant anastrozole and then relapsed. Currently, there is very little data on treatment options in this setting. It’s kind of a “dealer’s choice” because there are no hard-and-fast rules.
There are multiple options including fulvestrant, exemestane and even tamoxifen — if the patient hasn’t seen it — because it’s obviously still a very useful drug. So the sequence is going to be all over the map for most folks.
— Stephen E Jones, MD
In a patient who has completed five years of adjuvant anastrozole, I use exemestane or fulvestrant. In my experience, patients tolerate the fulvestrant injections just fine. We have randomized data comparing fulvestrant versus anastrozole in patients who have already received tamoxifen, but the optimal sequence for using fulvestrant is still undetermined.
In choosing between exemestane and fulvestrant, I ask my patients whether they prefer an injection or a pill. If they have transportation problems, then I use an oral agent. However, for the Medicare population, these drugs are very expensive. If the patient does not have adequate insurance coverage and can’t afford them, then a monthly injection may be better. Compliance is also an issue to be considered when choosing between a daily oral agent and a monthly injection.
— Joanne L Blum, MD
I think fulvestrant is a great alternative for patients with hormone receptor-positive metastatic breast cancer. Personally, I tend to use it as second- or third-line hormonal treatment. Not that I know that it’s worse or better than the other drugs, but more because it came last.
— Ann Partridge, MD
Most clinicians consider fulvestrant a third-line therapy for patients who have failed tamoxifen and an aromatase inhibitor; however, clinical trials have shown fulvestrant is equivalent to anastrozole after tamoxifen failure. In a recently published European study comparing front-line fulvestrant versus tamoxifen, I did not view fulvestrant as inferior.
Click here to see image
In addition, a Phase III study is underway comparing fulvestrant to exemestane for second-line therapy. I do use thirdline fulvestrant, but I will use it first-line, particularly in women who can’t afford an aromatase inhibitor. In addition, I would estimate that approximately 40 percent of my patients prefer a monthly injection to taking a pill every day.
— Adam M Brufsky, MD, PhD
Use of fulvestrant in premenopausal women
I only utilize fulvestrant in premenopausal patients in conjunction with ovarian suppression. Particularly in the metastatic setting, we find that many patients will opt for an oophorectomy after ovarian suppression, and then we can treat them as postmenopausal.
— Stephen E Jones, MD
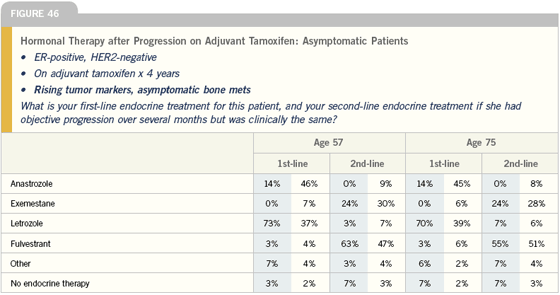
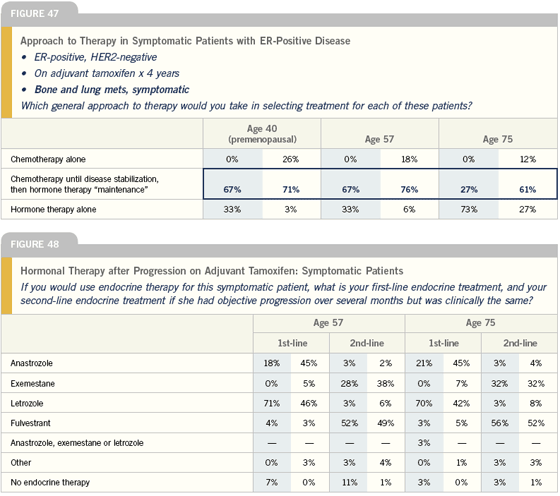
Management of symptomatic patients with ER-positive disease
Managing patients with ER-positive metastatic disease really depends on the symptoms. If the patient just has bone disease, I’m very likely to go with hormonal therapy, period, and control the bone pain. On the other hand, if she has extensive liver or lung metastases, I’m likely to use chemotherapy until disease stabilization and then bring the patient back to an aromatase inhibitor.
— Generosa Grana, MD
For a patient who has a pretty good amount of disease, chemotherapy is reasonable to recommend. The question comes up: Do you use chemotherapy alone in that scenario or do you combine it with hormonal therapy?
I think you have two opposing thought processes here. One is, if you go back to the olden days, 15 or 20 years ago, when they were looking at chemohormonal therapy versus chemotherapy or hormone therapy alone, the end result of using them together versus playing them out made no difference in survival.
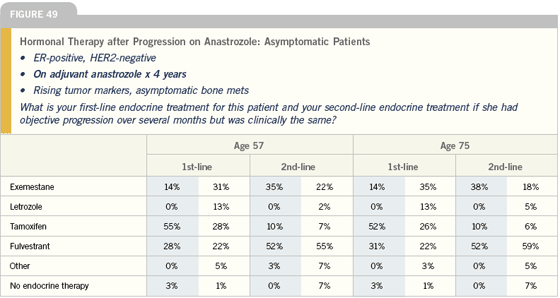
Click here to see image
But there was a higher response rate if you used them both together. So from that scenario, if you really need to get a response, going with chemotherapy combined with hormonal therapy makes sense. However, if you take into account Kathy Albain’s adjuvant data reporting that it’s best to give tamoxifen after the CAF, you could decide to separate the chemotherapy and the hormonal therapy.
I am not opposed to using them both together and would tend to do so. I would give the chemotherapy for two-six cycles, depending on how things were going and then stop it and stay with the hormonal therapy alone.
— Charles L Loprinzi, MD
Side effects and tolerability of fulvestrant
We have not had any problems administering fulvestrant injections. The newer double-doses being investigated for loading doses will require injecting five milliliters in each buttock, which may be an issue. It is a slow injection and the nurses just have to take their time. Most patients really don’t have any problem. The side-effect profile of fulvestrant is very benign — few menopausal symptoms and less chance of arthralgias than with aromatase inhibitors. Unlike tamoxifen, fulvestrant is not associated with a higher rate of thromboembolic side effects.
— Stephen E Jones, MD
I haven’t seen too many complaints with fulvestrant, but quite frankly most of these patients have been through so much by the time they get to fulvestrant, they’re not big complainers. They’re usually happy to be off chemotherapy. I know fulvestrant can cause hot flashes and menopausal symptoms, but I haven’t seen a whole lot of that. I have not used fulvestrant in a first-line setting yet.
— Ann Partridge, MD
My patients have tolerated the fulvestrant injections beautifully. They like the fact that they’re coming to the office only once a month. I keep asking them if they’re having significant injection site reactions, and I have not had any significant complaints.
Even the women who are on the loading dose, where they get two injections as part of a study, really have not had significant complaints.
— Generosa Grana, MD
Oral versus parenteral endocrine therapy for metastatic disease
I believe most patients, if they think the impact is same in terms of controlling their cancer and producing a response, will almost always opt for a pill. There are some specific ancillary situations where I think parenteral therapy has additional advantages to a woman who is paying for her pills out of pocket and doesn’t have to pay for an injection, one who has real compliance issues or one who can’t get back and forth for to the pharmacy to get refills.
However, if I mention that there are oral agents available, women will almost always jump at that opportunity. If they don’t tolerate the oral agents or the disease progresses, certainly, I will consider falling back on parenteral therapy, but up front, I generally go to an oral agent as my first hormonal manipulation in the metastatic setting.
— Gary Lyman, MD, MPH
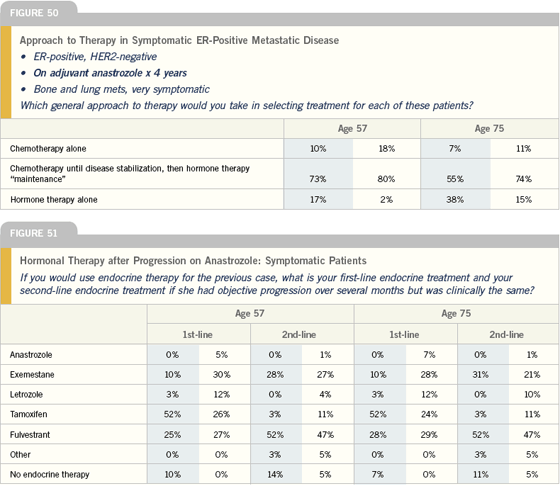
Click here to see image

I give my patients the option usually for second-line therapy and most of them to date prefer a pill to an injection, although some people clearly prefer a shot. I had one woman with whom I was actually going to use adjuvant fulvestrant, because she refused any therapy and I thought she might think about an injection. I was at a loss for what to do with her because she said she’d never take a pill. I think it’s an effective drug that has a lot of potential as an alternative or as another option down the line.
— Ann Partridge, MD
Select publications
|

